Infants -
3 to 6 months
The pathway for infants in this age group differs from younger babies - compensatory movement patterns are more established and newborn feeding reflexes are no longer present. This age group also has exclusive access to Ireland's only frenuloplasty service under conscious sedation, avoiding the need for general anaesthetic.
Recognise your baby's symptoms?
At this age, feeding difficulties remain the most common presentation, but ongoing weight gain concerns, unresolved colic, and reflux that has not responded to other interventions are frequently presenting features. Select the symptom most relevant to your baby's experience.
- Infant · FeedingBreastfeeding pain→
- Infant · FeedingPoor or shallow latch→
- Infant · FeedingNipple damage or pain→
- Infant · DigestionReflux, colic and wind→
- Infant · GrowthSlow weight gain→
- Unique Service · Ireland's OnlyFrenuloplasty under conscious sedation (12 weeks - 6 months)→
Not sure which applies? View all symptoms by age group or book a free Concerns Call.
The pathway for 3 to 6 month olds
The pathway of care for this age group differs from younger infants. At 3 to 6 months, compensatory movement patterns are more established and newborn feeding reflexes are no longer present for us to work with. Helping your baby transition to normal feeding patterns - using the muscles as intended and building stamina - takes additional preparation time and support.
A baby with a tongue tie will have adapted to this restriction from before birth, developing strategies to feed that in turn create tension patterns throughout the body. You may have noticed your baby turns their head one way more than the other, or finds tummy time particularly difficult. These are signs of the whole-body compensation that accompanies restricted oral function.
The initial appointment will assess whether tethered oral tissues are present and evaluate your baby's feeding. A recommended treatment plan will be discussed with you at the end of this appointment.
Feeding Assessment
One of our feeding specialists, an International Board Certified Lactation Consultant (IBCLC), will assess how your baby is feeding. They will observe whether your baby is using the tongue to create suction and extract milk, or whether compensation strategies - tongue or lip compression, tongue thrusting, or jaw dropping - are being used to achieve milk transfer. Latch, position, and pacing will be assessed. If you are bottle feeding, advice on bottle type and flow rate may be provided.
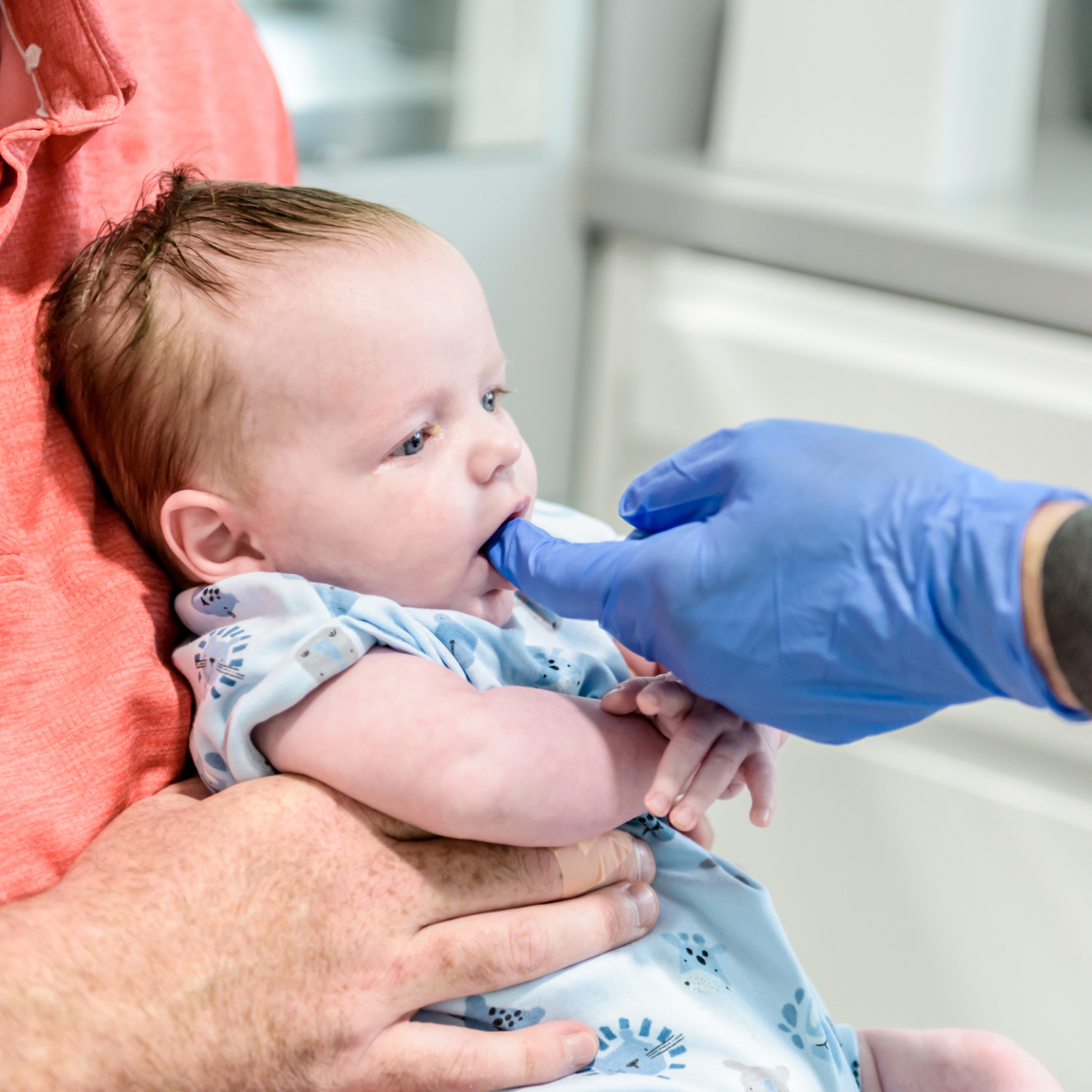
Medical Consultation
Dr. Justin Roche will examine your baby and discuss the findings of both the physical examination and the feeding assessment. A recommended treatment plan will be drawn up to prepare your baby for surgery where this is indicated. Surgery will be performed on a different day, allowing time for preparation to take effect.

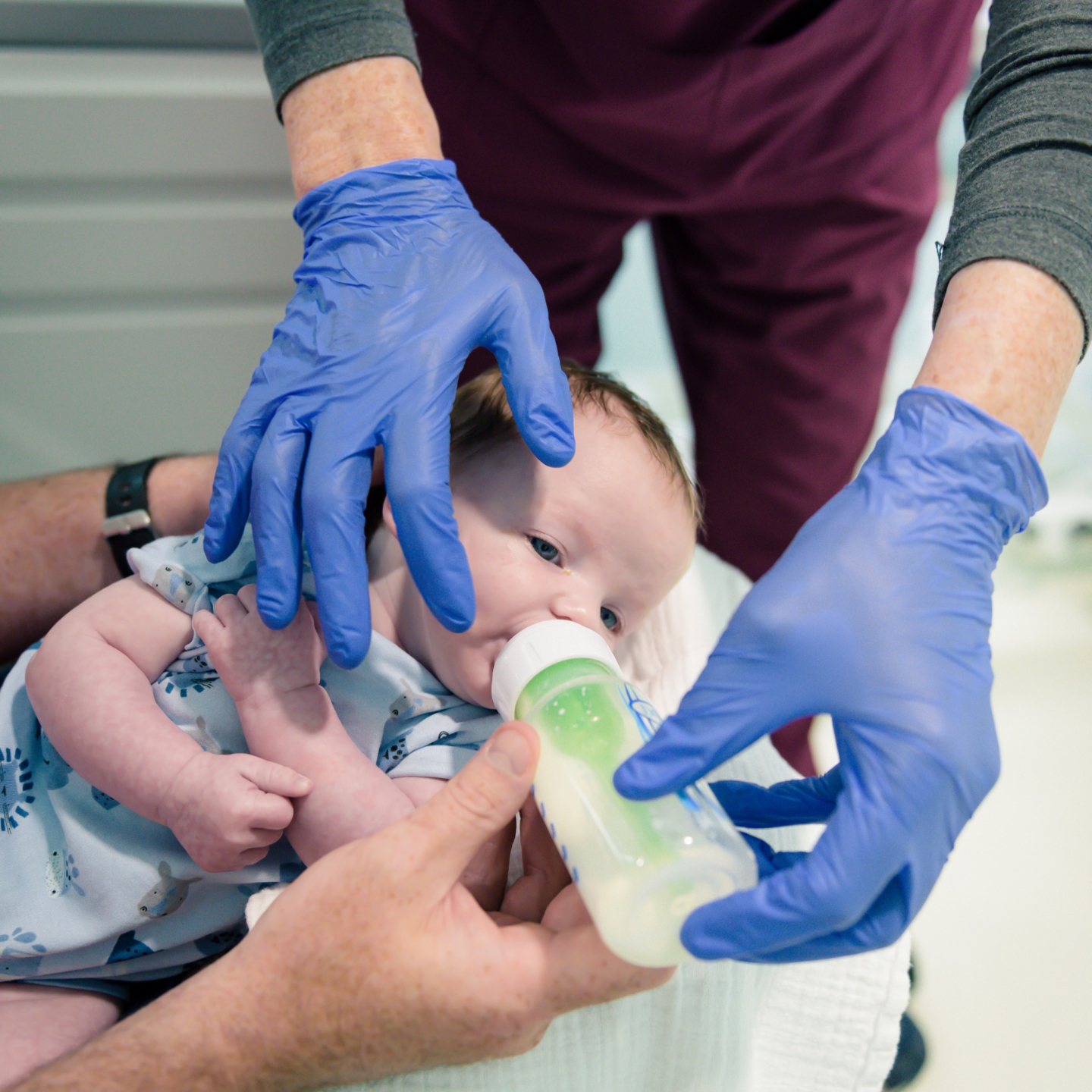
Pre-operative Feeding Support
Feeding support appointments are offered pre-surgery to help you and your baby prepare, giving the best chance of a successful outcome. You and your baby will be supported to begin working on the movement patterns and feeding mechanics that will be consolidated after the procedure. The number of pre-operative appointments depends on your baby's starting point and rate of progress.
Feeding Therapy
Feeding therapy is an appointment with a physiotherapist who has specialist training in infant feeding. This is recommended where a baby has a higher degree of oral dysfunction or additional challenges such as feeding aversion. It addresses the structural and functional aspects of the restriction from a physiotherapy perspective, complementing the lactation-led feeding support.
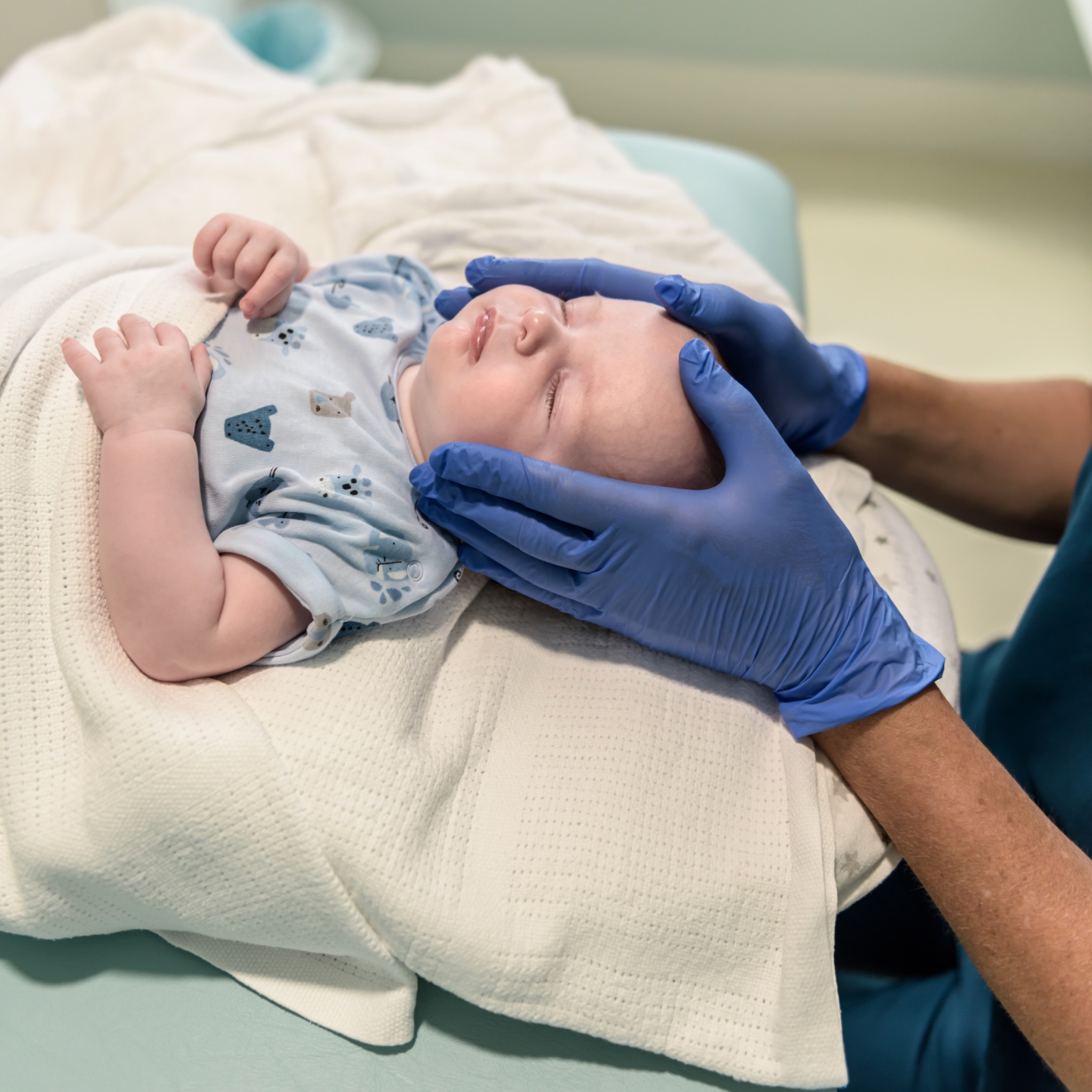
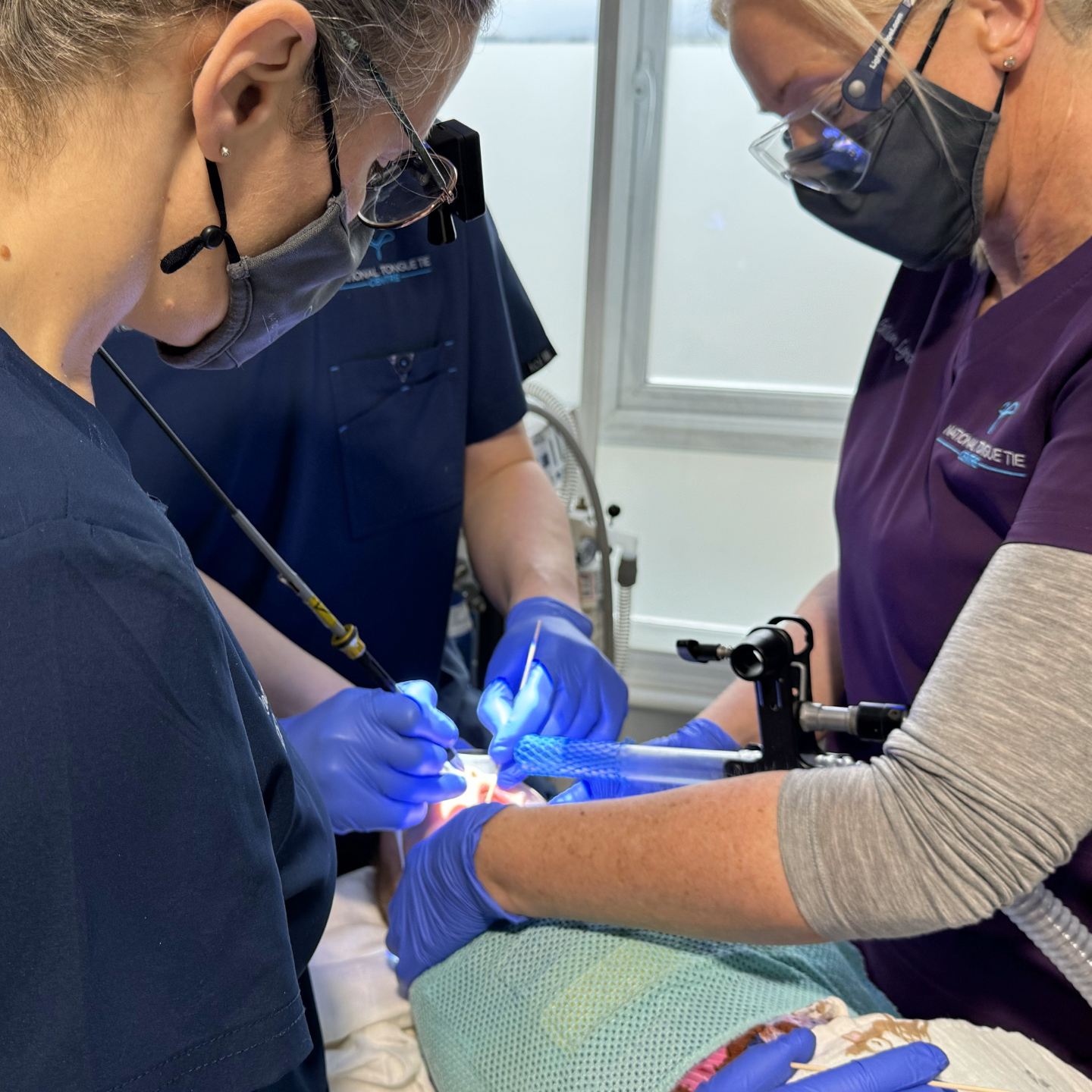
Functional Frenuloplasty under Conscious Sedation
Surgery is performed under conscious sedation - your baby will be breathing independently throughout and will have no memory of the procedure. They are kept comfortable by local anaesthetic numbing the base of the tongue, and monitored throughout using an ICU-grade monitoring system.
Because your baby is conscious during surgery, we can elicit tongue movements and assess muscle tone in real time. This allows us to gauge precisely how much fibrous tissue requires release for optimal function while creating minimal inflammation during healing. Doctor and physiotherapist work together in surgery. The surgical site is closed with absorbable sutures, meaning no active wound management is required at home post-operatively.
This approach is what differentiates a functional frenuloplasty from a release under general anaesthetic, where the patient is fully unconscious and muscles flaccid - removing the possibility of real-time functional assessment during surgery.
Post-operative Feeding Support and Therapy
The work begun pre-operatively is continued and monitored after surgery to achieve optimal healing of the surgical site, correct dysfunctional feeding patterns, and support habituation of normal movement patterns. You will be offered post-operative feeding support appointments in the days following surgery. The number of appointments depends on your baby's response to treatment and rate of progress.

Post-operative Medical Follow-up
Dr. Roche will arrange a follow-up appointment approximately eight weeks after surgery to confirm that the sutures have been fully absorbed, assess the healed surgical site, and review overall progress.
Common questions from parents
If you don't find what you need here, our free Concerns Call is the best next step.
Why is the pathway different for this age group compared to younger infants?
By 3 to 6 months, compensatory feeding patterns are more established and the newborn feeding reflexes we can use in younger infants are no longer present. This means more preparation time is needed to achieve the same quality of outcome. The pathway is longer, but the goal is the same: optimal long-term oral function, not just short-term symptom relief.
What is the conscious sedation service and why is it only available at NTTC?
Conscious sedation means your baby will be breathing independently throughout the procedure and will have no memory of it. This avoids the risks associated with general anaesthetic and allows us to assess tongue movement and muscle tone in real time during surgery, improving precision. To our knowledge, this service for infants aged 12 weeks to 6 months is currently unique to the National Tongue Tie Centre in Ireland.
How many pre-operative appointments will my baby need?
The number varies depending on your baby's degree of oral dysfunction and rate of progress. We will give you a realistic estimate at the initial assessment appointment once we have assessed your baby's specific situation. Our priority is ensuring your baby is genuinely ready for surgery, not simply meeting a number of appointments.
My baby was assessed at birth and told tongue tie was not significant. Should I get a second opinion?
If your baby continues to have feeding difficulties, unresolved reflux or colic, or is not gaining weight as expected, a specialist assessment is warranted regardless of previous assessments. Tongue tie assessment is a clinical skill that varies significantly between practitioners. We will assess your baby's current functional status and give you an honest opinion.
What is feeding therapy and how is it different from feeding support?
Feeding support is provided by an IBCLC and focuses on the lactation and feeding mechanics aspects of care - latch, position, technique, and milk transfer. Feeding therapy is provided by a physiotherapist with specialist training in infant feeding and addresses the oral motor and structural aspects of dysfunction, including oral sensitivity, tone, and movement patterns. For many babies in this age group, both types of appointment are part of the pathway.
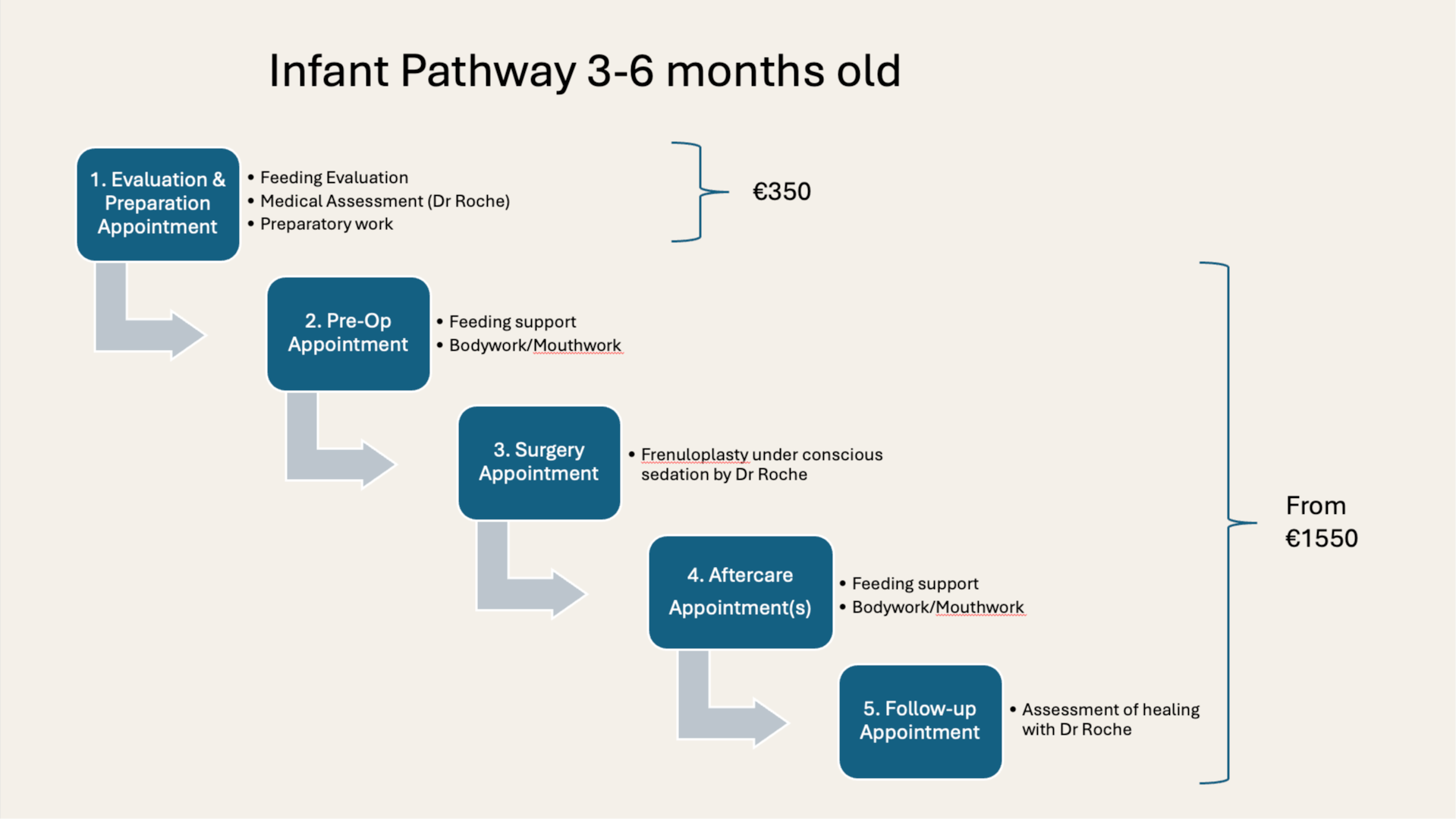
Transparent fee structure
The initial evaluation is a standalone appointment. You are not committing to any procedure by attending, and the clinical findings and feeding advice from this appointment are valuable regardless of whether you proceed to surgery.
Feeding assessment, medical consultation, and preparation guidance. No obligation to proceed.
Pre-operative feeding support, frenuloplasty under conscious sedation, and post-operative therapy and follow-up.
A payment plan is available. If you hold private health insurance, please see our fees page for information on coverage. Contact us if you need documentation to support a claim.
Ireland's original dedicated tongue tie clinic
Established in 2007 as Ireland's first clinic dedicated entirely to the assessment and treatment of tongue tie. Led by Dr. Justin Roche (Consultant Paediatrician, FRCPCH, FRCPI, IBCLC) and Kate Roche (Chartered Physiotherapist, IBCLC, Feeding Therapist). Clinics in Clonmel, Co. Tipperary and Naas, Co. Kildare.
Ready to get answers for your baby?
If your baby continues to have feeding difficulties, unresolved reflux or colic, or you are not satisfied with previous assessments, a specialist evaluation will give you a clear clinical picture. We will tell you honestly what we find and what, if anything, we recommend.
Clinics in Clonmel, Co. Tipperary and Naas, Co. Kildare. Patients seen from across Ireland and internationally.
Frenuloplasty is a surgical procedure. Risks, benefits, and individual expectations are discussed in full at assessment before any decision to proceed is made. The conscious sedation service is provided where clinically indicated following comprehensive assessment.

