Kate & Justin Roche • Co-Founders
Our Story

Kate and Justin, England, late 1990s
Our first introduction to tongue tie was twenty-seven years ago, when we became parents for the first time. We had both been working on the neonatal unit in Southampton, and when our eldest daughter was born, we were lucky enough to be able to call on people we trusted. When she had lost 10% of her birth weight by day five, lactation consultant Carolyn Westcott came to us, identified tongue tie, and paediatric surgeon Mervyn Griffiths released it the same day. She went on to breastfeed for a year. We didn't know what we didn't know, and so tongue tie did not cross our minds again for some time.

Southampton, April 1999
Learning Through Our Own Children
We have six wonderful children. Each one taught us something different, including many lessons learned retrospectively, when it came to our tongue tie journey.
Our second daughter had colic. The relentless kind. She gained weight, she was not unwell, and so there was no pathway to follow. When a baby has a temperature or is clearly unwell, you know what to do. A baby who has been fed, changed, held, and still cannot settle sits outside that framework entirely. We did not look for a clinical explanation because nothing pointed us toward one. We assumed we were not coping well enough. We put it down to the circumstances of life with a new baby (and another house move) and got through it. It was only much later that we understood her tongue tie had been part of that picture all along.
Our third child showed us what straightforward feeding looks like. We had not known, until then, what that felt like.
Our fourth child was labelled failure to thrive, which now would be called faltering growth or weight. What followed was months of hospital visits and an admission for investigations: overnight pH studies, a barium swallow, a sweat test to rule out cystic fibrosis, and an eventual diagnosis of gastro-oesophageal reflux disease. He was placed on proton pump inhibitors. He continued to vomit significantly throughout his first year. He was so orally defensive from the experience that he refused spoon feeding entirely, which is how we came to baby-led weaning, out of necessity rather than philosophy. We know that the investigations he had were standard practice. We now know that what he needed was someone to recognise that his oral function was the root of it. That person did not exist in the system he entered. He needed us, and we were not yet ready.

He needed us, and we were not yet ready.
"I remember the tears. His tears after every feed. My tears when we put him on the scales and the numbers had gone down despite feeding all day. And tears even years after, when I would come across a baby photo and feel like we had failed him."
The Turning Point
Our fifth baby was born when we were living at the foot of the Wicklow Hills. Feeding difficulties were immediate and significant. We contacted lactation consultant Nicola O'Byrne, who suspected tongue tie, but back then, she told us there was nobody in Ireland who would treat it. We contacted Carolyn Westcott in Southampton, who gave us a clear choice: get on a plane, or manage this ourselves. Faced with no other option, we did it ourselves. Justin performed a scissors release with me assisting. Things improved, but not enough. Eventually we persuaded a paediatric surgeon at Crumlin Children's Hospital in Dublin to complete the posterior component of the release. That required a general anaesthetic and an overnight hospital stay. But it made a difference that mattered. For the first time, she could transfer milk effectively. She could feed.

Life was busy but we now had a baby who could feed.
Once he saw the difference it made to our own child, Justin could not unsee it when looking after babies in his daily work. So he returned to Southampton and trained with Mervyn Griffiths, the same paediatric surgeon who had treated our eldest daughter years before. He came back equipped. When you know how to make things better, not acting is no longer an option. He was working as a Consultant Paediatrician in Tipperary and began treating babies in the hospital as he encountered them. Word spread and before long a lactation consultant in Limerick was ringing to ask could she send a mother and baby. That was when the day ward in Paediatrics became involved, and a service that had begun with our own children started to grow.
Building the Service
As the service expanded, with parents starting to travel from all over Ireland, the paediatric nurses, quite reasonably, pointed out that the day ward simply did not have the space. Mothers feeding, babies, buggies everywhere. Justin moved to outpatients. The public clinic continued to grow, and when the waiting list became too long to manage, we started a private clinic alongside it. Friday evenings first. Then Saturdays. Then Sundays. We had to work out of hours to have the space to allow time for feeding with no pressure on families.
Lactation consultant Claire Bulfin contacted us to offer her services. She brought two further lactation consultants with her, and from that point on every family who came to us was seen by a lactation consultant as part of their care. That was the shift that turned what Justin and I had been doing on our own into building a team. Claire was central to the development of those early years, and the multidisciplinary model we are known for today was built on the foundation she helped us lay.
But we were still running out of space, and we knew that to do this properly, we needed somewhere of our own.
January 5th, 2017
During the recession that followed the Celtic Tiger, we had converted part of our home into accommodation for medical students on placement. One afternoon, I was preparing those rooms, racking my brains about where we might find four consulting rooms, a waiting area, and a procedure room in Clonmel. Standing in the fourth bedroom, it occurred to me that I was already in it.
The medical students got moved on and the space was converted yet again. On January 5th 2017, the National Tongue Tie Centre opened. Fr Bobby arrived to bless the clinic while Claire was outside on the driveway with a power washer, clearing the mud left by the diggers who had just finished the car park. Chaos, but the start of a new era.
We built what we had needed all those years ago. When you arrive, you are not walking into a hospital. You arrive to a garden where you can breathe, where children can run free after a long journey. The mountains are visible. There is coffee on. A team equipped to help. The space is designed to say: you are welcome here, you are heard here, you are supported. We had been those parents. We knew what was needed.
"Every family deserves to enjoy their baby. Every child and adult deserves to function without compensating. Why make life harder than it needs to be?"
The Learning Continues
We never stop learning. As we began treating older children and adults, it helped us understand the full consequences of either not treating tongue tie at all, or not treating it to an optimal standard. Seeing the sequelae across a lifetime, the skeletal challenges, the breathing issues, the postural compensations, gave us a clarity about infant treatment that we could not have had otherwise. And as we began seeing patients who had already had surgery elsewhere, sometimes years earlier, we understood that surgery alone is not the fix. It might make things better. It does not automatically mean you achieve the optimal outcome for the lifetime ahead.

Six children. Six teachers.
That understanding was also deeply personal. We had taken it in turns in those early years, one of us staying with the children while the other flew, most often to the United States, for courses and conferences as we invested years in training. As our knowledge grew, so did our ability to look back at our own children with clearer eyes. Our eldest had gone on to breastfeed successfully for a year. We had considered that a good outcome. What we came to understand was that she had remained restricted, and that restriction had consequences: migraines, significant orthodontic requirements, challenges that emerged only later and that we had not connected to those early feeding days. That realisation shifted our thinking permanently. Function means everything. Not just feeding. Not just the early weeks. But the lifetime of breathing, sleeping, growing, and thriving that follows. Surgery is one part of that. Optimal function is the goal. We treated three of our children in their early teens who we had missed as babies. We are also now blessed with two grandchildren who also had tongue tie and so our learning continues.
It also turns out that when you spend decades immersed in this field, your own extended family becomes something of an unwitting case study. Looking across the generations, we began to see the same patterns repeating. The same craniofacial features, the same sleep difficulties, the same orthodontic histories, the same unexplained health challenges that nobody had ever thought to connect. My father is a keen photographer, and his archive reaches back to the late 1800s. Looking back through those photographs, across parents, grandparents, and great grandparents, we can trace the craniofacial features associated with oral dysfunction across generations: the open-mouth posture, the shadows beneath the eyes, the narrow facial growth patterns. It was there all along, hiding in plain sight, entirely unrecognised for what it was. This is not a modern problem. It is an ancient one that we are only now learning to read.
We have also come to understand how unresolved oral dysfunction can shape a lifetime. Poor sleep across the middle years has well-documented effects on cognitive function in later life. My mother has Alzheimer's. Sleep was always a problem for her. We cannot say with certainty that these things are connected, but we believe it played a role.
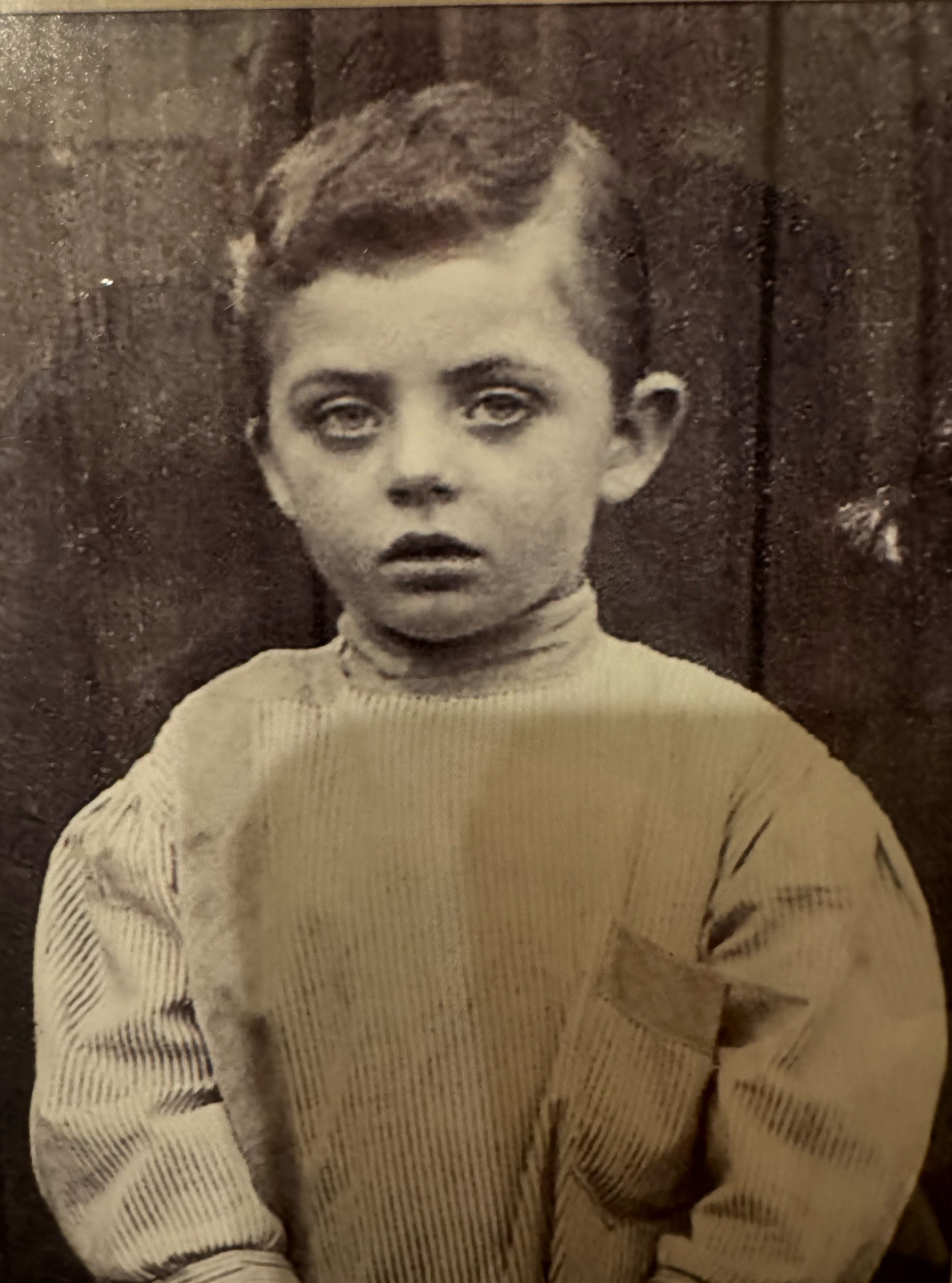
My Great Grandfather.
We have also been shaped by loss within our extended family that we carry quietly. It has contributed to the urgency with which we work, and to the care we take with every family who comes through our door.
Why We Do What We Do
The National Tongue Tie Centre now sees over 1,000 patients annually. Families travel to us from across Ireland and also from abroad. We have an amazing team of skilled clinicians and dedicated support staff trained to the same clinical standard we hold ourselves to. We have continued to develop our methodology, our multidisciplinary approach, our understanding of prehabilitation, full functional release, rehabilitation, and the lifelong impact of optimal oral function on breathing, sleep, craniofacial development, swallowing, and posture.
The Functional Frenuloplasty technique was developed by Dr. Sourish Zaghi. Justin has brought this procedure to babies and children, pioneering the routine use of conscious sedation for tongue tie surgery in children from 12 weeks to 12 years, making this option accessible where previously it had not been. His ongoing clinical work has focused on selective fascial release as an integral part of that approach. I bring my experience in physiotherapy, lactation, craniosacral therapy and feeding therapy to create an integrated clinical lens through which to meet the individualised needs of our patients. Together, we present internationally, help set standards of care, and continue to push the boundaries of what this field can offer.
But the reason we come in every day is simpler than any of that. It is the couple sitting in our waiting room, struggling and exhausted, who have been told there is nothing wrong. It is the baby who deserves the chance to feed well, sleep well, and grow well. It is the family who deserves to enjoy those early months instead of surviving them.
We have been that family. We know what it costs when the right help is not there. We have spent the last twenty or so years making sure it is.
"Good enough is not good enough. Every child and adult deserves optimal function. That is why we are here."
Our journey, our learning, and our passion for this work continues every day. Follow along.
Kate and Justin Roche
Co-Founders, National Tongue Tie Centre
Clonmel, Co. Tipperary
www.tonguet.ie
Our children grew up watching us chase answers and they continue to push us to do better. See us all working together in the photos below. The learning never stops.
1 / 11











